A Triple Breakthrough for Maternal Health and HIV Care: What it Means for Africa
Written By Maxine Ansah
|
Getting your Trinity Audio player ready...
|
In a landmark move to advance global health goals, the World Health Organization (WHO) has announced several updates with far-reaching implications for African countries. These updates span new rapid diagnostic tools, guidance on HIV disclosure for children and adolescents, and recommendations on HIV care linked to mpox. Together, they promise to strengthen prevention, diagnosis and treatment across the continent.
First triple rapid test prequalified for HIV, hepatitis B and syphilis

On 10 July 2025, WHO prequalified the first bundled rapid diagnostic test capable of simultaneously detecting HIV, hepatitis B virus (HBV) and syphilis. Known as the Determine™ Antenatal Care Panel, this point-of-care test uses a simple finger-prick blood sample to deliver quick, qualitative results.
These three infections remain leading causes of preventable illness and death and carry a significant risk of mother-to-child transmission during pregnancy, childbirth or breastfeeding. Early detection is vital. Timely testing enables pregnant women to access treatment and preventive measures, drastically lowering the risk of passing infections to their infants.
Dr Rogério Gaspar, Director of WHO’s Department of Prequalification and Regulation of Medicines and Health Products, said:
“Ensuring rapid access to quality-assured diagnostic tests is essential to protecting the health of vulnerable populations, including pregnant women”.
For African countries, where health systems often face resource constraints and antenatal testing coverage remains uneven, this development could transform maternal and child health services by making integrated, efficient testing more accessible.
New guidance supports HIV disclosure for children and adolescents

WHO has also released updated guidance to help children and adolescents living with HIV understand and safely share their HIV status. This update is the first practical resource since WHO’s earlier guidance published in 2011.
Disclosure, when managed thoughtfully, can improve mental health, social support and adherence to treatment, leading to better clinical outcomes. Yet it remains a complex process for families and health providers.
Nicola Willis, Executive Director of Zvandiri, a Zimbabwean community-based organisation, explained:
“All children and adolescents have the right to and need for information that helps them make sense of their world. This new guidance reminds us that discussing their HIV status with them is an essential component of their treatment and care”.
The guidance outlines evidence-based approaches to disclosure, taking into account developmental stages, stigma, family communication and support systems. By providing clear examples and recommendations, it aims to help health workers, policymakers and caregivers support young people living with HIV more effectively.
Rapid ART recommended for people living with HIV diagnosed with mpox
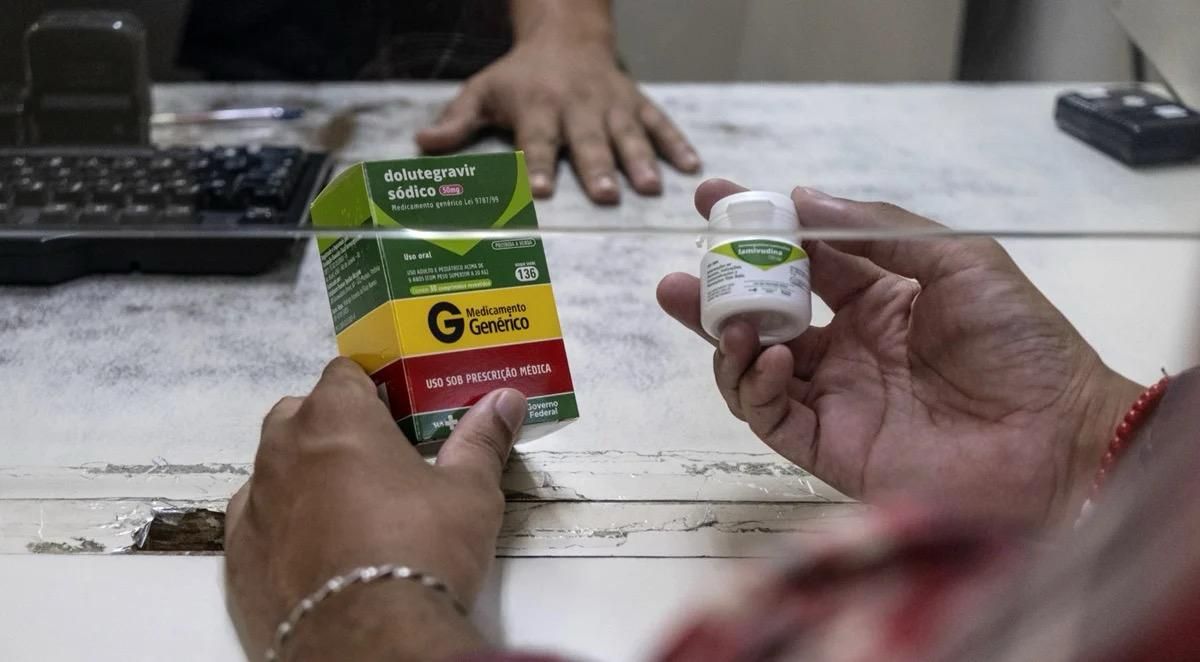
In a further update, WHO now strongly recommends the rapid initiation of antiretroviral therapy (ART) for people living with HIV who are diagnosed with mpox, previously known as monkeypox.
Mpox can be more severe in people with advanced HIV disease, leading to higher hospitalisation and mortality rates. WHO experts concluded that starting ART quickly – ideally within seven days of HIV diagnosis, including same-day initiation where possible – outweighs potential risks linked to immune reconstitution inflammatory syndrome.
Dr Meg Doherty, Director of WHO’s Global HIV, Hepatitis and STI Programmes, noted:
“We now know people with HIV, particularly those with a CD4 count under 200 cells/mm³, are at risk for severe disease and death from mpox”.
This recommendation complements WHO’s broader push for integrated HIV care, including early HIV and syphilis testing for those with suspected or confirmed mpox.
Moving towards integrated, people-centred health care
These updates come as many African countries work to integrate HIV, hepatitis and sexually transmitted infection services into primary healthcare systems. A recent WHO policy brief documents lessons from countries such as Kenya, Botswana and Rwanda, which have shown that coordinated and community-focused strategies can improve service delivery and health outcomes.
Rapid multiplex testing, better disclosure support, and faster treatment initiation are all tools that can help African countries close gaps in prevention and care. Dr Meg Doherty summarised this potential, saying:
“Rapid multiplex tests like this mark a new era for diagnostics as they have potential to transform service delivery and population health”.
Turning innovation into action remains the challenge. Yet, with these new tools and guidance, African health systems are better equipped than ever to protect women, children and communities.


