|
Getting your Trinity Audio player ready...
|
UNAIDS has hailed the United States State Department’s announcement that PEPFAR, the President’s Emergency Plan for AIDS Relief, will support the Global Fund’s initiative to deliver lenacapavir, a twice-yearly HIV prevention drug, to up to two million people in countries with high HIV burdens. This extraordinary medicine, a long-acting injectable, promises to transform HIV prevention for those most at risk. UNAIDS, however, urges the world to aim higher, to ensure that in time, everyone in need can benefit from this breakthrough.
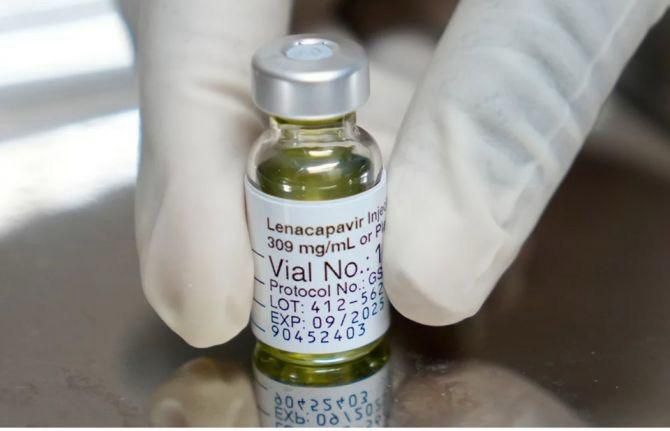
Lenacapavir, developed by Gilead Sciences and administered only twice a year, stands to change lives. Its potential to reach populations that have been left out, young women and adolescent girls, sex workers, people who inject drugs, and men who have sex with men, is immense. For African nations where HIV remains a devastating reality, this injection brings a fresh chance at turning the tide of the epidemic.
UNAIDS underscores that the initial roll-out of two million doses is a strong start, but not enough. An estimated twenty million people globally will ultimately require antiretroviral-based prevention tools such as lenacapavir to meet the 2030 HIV prevention targets. The economic upside is clear: every dollar invested in prevention could save seven in future treatment costs, making the case for urgent and scaled-up action.
Until recently, lenacapavir came with a daunting price tag, over US$28,000 per person per year in countries like France, Norway, Spain and the United States. Under this new initiative, Gilead has committed to supply the drug at no profit. Research shows it can be manufactured and offered for about US$40 per person per year, potentially falling to US$25 when produced at scale.
For African countries, the implications are profound. Nations such as South Africa, Kenya, Uganda and others bear the brunt of the global HIV burden and urgently need affordable and effective prevention tools. Lenacapavir’s simplicity, just two injections yearly, could dramatically improve adherence, ease logistical burdens on health systems, and reduce the stigma associated with daily pills. Girls and young women, who often face the highest infection rates, stand to benefit enormously.
Gilead’s strategy accelerates access: it has launched voluntary licensing agreements with six generic manufacturers, enabling supply to 120 high-incidence, resource-limited countries. Regulatory steps are already underway, including submissions in 18 priority countries across Africa that account for roughly seventy per cent of this HIV burden. WHO prequalification and EU M4all approvals are expected this year, enabling speedy local regulatory authorisations.
Yet to succeed in Africa, community engagement must be central. UNAIDS rightly stresses that people most affected by HIV must shape the roll-out. If implemented with sensitivity to local contexts, lenacapavir could close critical gaps in prevention, saving lives, empowering communities, and accelerating progress toward ending AIDS as a public health threat by 2030.
This announcement is not just a dose of medicine; it is a dose of ambition. Africa may finally be witnessing not just incremental progress but a turning point in the HIV response. The challenge now is to ensure this momentum reaches every person who needs it.